Apex Addiction Recovery Center operates two treatment facilities across Tennessee; today, we’re going to focus on Tennessee. Our presence in Tennessee ensures accessible and comprehensive treatment options for people seeking rehab support. Apex Substance Addiction Recovery Center is the trusted partner for anyone looking for a path to sobriety in the Volunteer State.
Apex Recovery operates treatment facilities in middle Tennessee. We’re proud to be in-network with numerous health insurance providers, ensuring accessible care for those seeking treatment. Specifically, we accept insurance plans from HealthNet, providing those in need with comprehensive coverage options for their recovery journey.

Who is Health Net Insurance Provider?

Health Net Insurance Provider is a prominent American health insurance company, known for offering an extensive range of health insurance products and services to meet the diverse needs of its members. With a commitment to delivering comprehensive and accessible healthcare solutions, Health Net is a trusted name in the health insurance industry, catering to individuals, families, and businesses.
Founded in 1977, Health Net’s offerings include a variety of health plans and services such as HMO, PPO, Medicaid, and Medicare Advantage plans. Their mission is to help people be healthy, secure, and comfortable. Health Net has a strong presence in the U.S. market, providing tailored healthcare solutions that emphasize preventive care and wellness, alongside a wide network of healthcare providers to ensure members receive the care they need.
Some of Health Net Brands, Products and Services in Tennessee
Health Net offers a variety of brands, products, and services tailored to meet the healthcare needs of individuals and families in Tennessee. Some of their offerings in the state include:
- Health Net CommunityCare: This program provides Medicaid managed care services, offering comprehensive healthcare coverage to low-income individuals and families.
- Health Net Individual and Family Plans: Tailored health insurance plans designed for individuals and families who are not covered by employer-sponsored insurance, providing access to a wide network of healthcare providers.
- Health Net Medicare Advantage Plans: Medicare Advantage plans offering comprehensive healthcare coverage for seniors, including medical, prescription drug, and additional benefits such as dental and vision care.
- Health Net Dental Plans: Affordable dental insurance options providing coverage for preventive, basic, and major dental services, helping members maintain good oral health.
- Health Net Vision Plans: Vision insurance plans offering coverage for routine eye exams, eyeglasses, and contact lenses, ensuring members have access to essential vision care services.
Drug and Alcohol Addiction Treatment Statistics in Middle Tennessee
In Tennessee, the opioid crisis continues to pose significant challenges, with over 3.3 million opioid painkiller prescriptions dispensed in 2022. Alarmingly, the state witnessed nearly 21,000 nonfatal overdose outpatient visits and more than 7,000 nonfatal overdose inpatient stays in 2021 alone. Tragically, 3,814 people lost their lives to drug overdoses in Tennessee in the same year.
Statistics also reveal concerning rates of substance use disorders, with 5.9% of people aged 18-25 experiencing Illicit Drug Use Disorder, 4.3% experiencing Alcohol Use Disorder, and 6.5% with Substance Use Disorder statewide. The stark increase in drug overdose death rates, rising from 17.2 per 100,000 people in 2011 to 56.6 per 100,000 people in 2021, highlights the gravity of the situation in Middle Tennessee compared to the national average of 32.4 per 100,000 people in 2021.

Free Addiction Assessment
Schedule a free, confidential assessment with a licensed clinician. Apex Recovery can check your insurance coverage levels for drug and alcohol addiction, and mental health treatment.
What is Health Net Rehab Insurance Coverage in the Volunteer State?
In the Volunteer State, Health Net Rehab in TN Insurance coverage offers specialized plans designed to support those seeking rehabilitation services. These plans cater to a wide range of rehabilitation needs, including physical therapy, substance abuse treatment, and mental health services. Health Net ensures that residents of Tennessee have access to the necessary care for recovery and wellness.
Health Net’s comprehensive approach to rehab insurance in Tennessee includes a variety of treatment options, from inpatient care and outpatient care facilities to counseling and therapy sessions. Through their network of qualified healthcare providers, Health Net facilitates access to high-quality rehabilitation services, supporting the health and well-being of Tennesseans on their journey toward recovery. See our insurance page for more information.
Does Health Net Cover Substance Addiction Rehab in Tennessee?
So, does Health Net cover rehab in TN? Yes, Health Net often provides coverage for substance addiction rehab in Tennessee. This includes a range of treatments for substance abuse, from detoxification and inpatient rehab to outpatient programs and counseling, ensuring members have access to vital support for recovery.
Health Net’s coverage is designed to meet the diverse needs of those battling addiction, offering access to an extensive network of specialized providers in Tennessee. By covering services like behavioral therapy, medication-assisted treatment, and ongoing support groups, Health Net helps to facilitate a holistic approach to recovery.
Does Health Net Cover Medical Detox Services in TN?
Yes, Health Net generally offers medical detox services in Tennessee. Medical detoxification is a crucial first step in the treatment of substance addiction, helping people safely manage withdrawal symptoms under medical supervision. Health Net’s coverage for medical detox services typically includes access to licensed detoxification facilities staffed by medical professionals trained to provide personalized care.
These services may involve medications to alleviate withdrawal symptoms, monitoring of vital signs, and supportive therapies to ensure the safety and comfort of patients undergoing detoxification. By covering medical detox services, Health Net helps support people in Tennessee as they begin their journey toward recovery from substance addiction.
Does Health Net Cover Residential Rehab in TN?
Health Net typically covers residential rehab services in Tennessee. Residential rehab, also known as inpatient treatment, provides a structured environment where people can focus solely on their recovery from substance addiction under 24-hour supervision. Its coverage for residential rehab typically includes room and board, medical care, therapy sessions, and access to various tailored treatment modalities.
Health Net alcohol rehab in TN supports people in Tennessee who require intensive, round-the-clock care to overcome addiction and achieve long-term sobriety. This comprehensive coverage shows Health Net’s commitment to providing access to quality addiction treatment services for its members in the state.
Does Health Net Cover Dual Diagnosis Treatment?
Health Net does typically cover dual diagnosis treatment in Tennessee. Dual diagnosis treatment addresses co-occurring mental health disorders and substance abuse issues, providing integrated care to address both aspects of a person’s health. Health Net’s coverage for dual diagnosis treatment typically includes comprehensive assessments, psychiatric consultations, medication management, individual and group therapy sessions, and ongoing support services.
By covering dual diagnosis treatment, Health Net ensures that Tennesseans receive holistic care addressing both their mental health and substance abuse concerns, promoting better outcomes and long-term recovery.

Other Rehab Treatment Programs Covered by Health Net in Tennessee
Health Net in Tennessee offers a variety of rehab treatment programs, ensuring members have access to a variety of care levels fit to their recovery needs. From structured, hospital-like settings to flexible outpatient models, Health Net’s coverage extends to Partial Hospitalization Programs, Intensive Outpatient Programs, and traditional Inpatient Rehab, each designed to facilitate a path to recovery.
Health Net Coverage for Partial Hospitalization Programs in TN
Partial Hospitalization Programs (PHP) in Tennessee offer intensive, structured treatment for substance abuse or mental health disorders. Participants attend sessions during the day, typically for several hours, receiving therapy, medication management, and other support services while returning home in the evenings. PHPs provide a level of care that is more intensive than outpatient programs but less restrictive than inpatient treatment.
Health Net typically covers Partial Hospitalization Programs in Tennessee, recognizing their effectiveness in addressing substance abuse and mental health issues. By providing coverage for PHPs, Health Net makes sure that its members have access to comprehensive and personalized treatment options that support their recovery path.
Health Net Coverage for Intensive Outpatient Program in TN
Intensive Outpatient Programs (IOP) in Tennessee are designed for those seeking recovery from substance abuse or mental health conditions who don’t require round-the-clock supervision. IOP allows participants to engage in their daily lives—attending to work, school, or family duties—while participating in scheduled treatment sessions. These programs focus on therapy, counseling, and education about substance use and mental health.
Health Net typically provides coverage for Intensive Outpatient Programs in Tennessee. This coverage allows access to vital therapeutic services, enabling members to pursue their recovery while managing their personal and professional responsibilities.
Health Net Coverage for Inpatient Rehab in TN
Inpatient Rehab programs in Tennessee offer intensive, round-the-clock care for people struggling with substance abuse or mental health disorders. Participants reside in a structured facility for the duration of the program, typically ranging from a few weeks to several months, receiving comprehensive treatment and support from a multidisciplinary team.
Health Net generally covers Inpatient Rehab programs in Tennessee, understanding the critical role they play in facilitating lasting recovery from substance abuse and mental health conditions. This coverage ensures that people have access to the intensive, comprehensive care they need to address their challenges and work towards sustainable wellness.
- Please complete and send the form below.
- One of our staff members will contact your insurer to check your coverage.
- We will contact you promptly with the results and to discuss the next steps.
Insurance Verification
"*" indicates required fields

Rehab Center in Tennessee That Takes Health Net
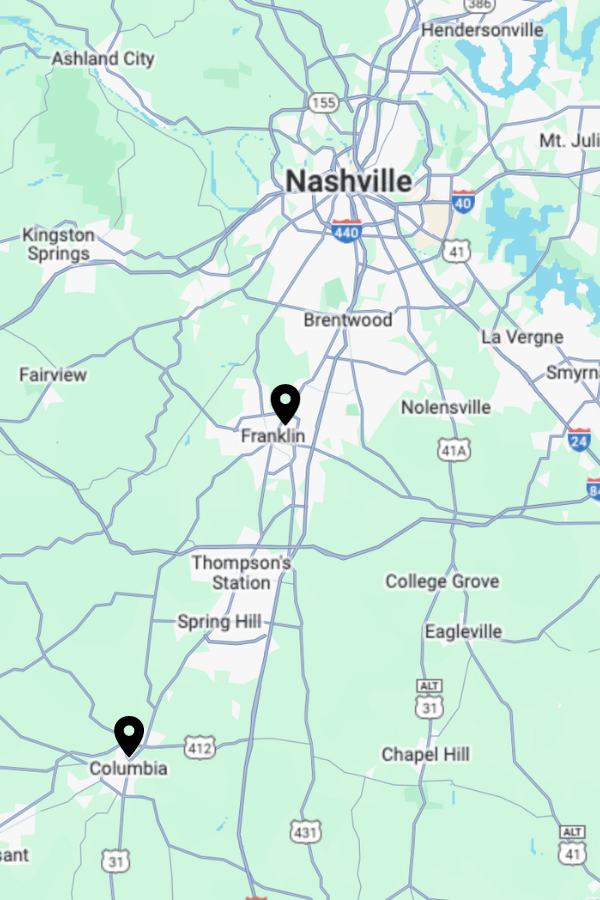
If you need Rehab centers that take Health Net in TN, Apex operates two premier facilities in Tennessee. Apex in Franklin and Apex in Columbia, provides accessible, high-quality care. Call us at (877) 881-2689 today.
Apex Recovery Franklin
4601 Carothers Pkwy STE 250A
Franklin, TN 37067
Apex Recovery Columbia
2710 Trotwood Ave STE A & B
Columbia, TN 38401

What is the Distance of Apex Rehab Tennessee Locations to Local Major Cities?
Apex Addiction Recovery Center in Tennessee offers convenient access to major cities across the state, facilitating ease of travel for those seeking rehabilitation services. Situated in Franklin and Columbia, these facilities provide comprehensive care within proximity to key urban centers, ensuring accessibility for residents across Tennessee.
Here are the approximate distances from some of the major cities to Apex Alcohol and Drug Addiction Recovery Centers:
- Nashville: Franklin is about 20 miles south of Nashville, TN.
- Memphis: Franklin is approximately 200 miles northwest of Memphis, TN.
- Knoxville: Franklin is around 180 miles east of Knoxville, TN.
- Chattanooga: Franklin is roughly 150 miles southeast of Chattanooga, TN.
Apex Drug and Alcohol Addiction Recovery Center’s locations make it feasible for people from various parts of the state to access their services with relative ease. Whether traveling from the bustling city of Nashville or the scenic landscapes of Chattanooga, Apex’s rehabilitation centers are conveniently situated to support those on their journey to recovery.
Popular and Familiar Attractions in Middle Tennessee
Middle Tennessee beckons with attractions like the historic Grand Ole Opry and Ryman Auditorium, the immersive Country Music Hall of Fame, and the natural splendor of Cheekwood Botanical Garden. Not to be missed, the architectural grandeur of The Parthenon is an interesting experience, while the savory allure of Nashville’s hot chicken offers a taste of local flavor.
Exploring Middle Tennessee and its Famous Towns
Located in the heart of the Volunteer State, Nashville is a vibrant hub, earning its name of Music City due to its deep-rooted connections to country music and the iconic Grand Ole Opry. Geographically, it’s a stone’s throw away from the undulating Appalachians to the east and the serene Tennessee River that carves through the state.
Beyond Nashville, Tennessee offers several notable cities—Memphis, the birthplace of the blues and the legendary Elvis Presley; Chattanooga, gatekeeper to the Great Smoky Mountains; and Knoxville, a gateway to the Appalachians. Each city has its unique allure, from the soulful strains of Memphis blues to the famous hot chicken and BBQ of Nashville.

Average Cost of Addiction Rehab in Tennessee with Health Net Insurance?
How much is rehab with Health Net Insurance in TN? The average cost of addiction rehab in Tennessee with Health Net insurance can vary depending on several factors in your individual policy. Typically, Health Net insurance helps alleviate a significant portion of the expenses of addiction rehab, including detoxification, therapy sessions, medical care, and other support services.
However, out-of-pocket expenses such as copayments, deductibles, and coinsurance may still apply, depending on the individual’s insurance plan. If you’re seeking Health Net drug rehab in TN, consult with the experts at Apex Substance Addiction Recovery Center to understand your coverage details and any potential financial responsibilities.
How to Check Health Net Coverage Levels for Rehab Treatment in Tennessee
To check Health Net coverage levels for rehab treatment in Tennessee, reach out to the experts at Apex Recovery. Call us at (877) 881-2689 or check your insurance here to obtain detailed information about your insurance benefits, coverage extent, and any applicable deductibles or copays specific to rehab treatment services. Contact us online anytime.
Take the time to verify insurance coverage at https://apex.rehab/verify-your-insurance/ before committing to our rehab programs to fully leverage your Health Net benefits while minimizing financial surprises. Apex Recovery facilitates this process, aiming to make access to crucial rehab services as smooth and informed as possible. By utilizing these resources, you can focus more on your recovery journey and less on the logistics of insurance coverage.
How to Get Health Net to Pay For Rehab Treatment in the State of TN
To get Health Net to pay for rehab treatment in Tennessee, you should start by contacting Apex. You can inquire about coverage options for rehab services and obtain details regarding any preauthorization requirements or documentation needed for reimbursement. We work with insurance providers and can clarify any questions you have.
The professionals at Apex can help navigate the insurance process, communicate with Health Net on your behalf, and ensure that all necessary steps are taken to maximize insurance coverage for rehab treatment in Tennessee. Contact us today.
How Many Times Will Health Net Insurance Pay for Rehab in Tennessee?
The number of times Health Net Insurance will pay for rehab in Tennessee can vary based on each person’s specific insurance plan and the benefits it includes. Generally, Health Net plans offer coverage for rehab services, but they might have limits on the number of treatment days, sessions, or program enrollments allowed.
To understand the specifics of how many times Health Net will cover rehab, members should contact Apex Addiction Recovery Center today. Customer service can provide detailed information about coverage limits, any potential restrictions, and the process for obtaining approval for rehab services. We offer assistance in working with insurance companies like Health Net to clarify coverage and advocate for the necessary treatment.

Drug and Alcohol Addiction Treatment Statistics in Tennessee (TN)
- There were more than 3.3 million opioid painkiller prescriptions in TN in 2022
- There were nearly 21,000 nonfatal overdose outpatient visits in the state in 2021
- More than 7,000 nonfatal overdose inpatient stays in 2021
- 3,814 people died in Tennessee from drug overdoses in 2021
- 5.9% of those aged 18-25 in Tennessee had an Illicit Drug Use Disorder
- 4.3% of those aged 12 or older in Tennessee had Alcohol Use Disorder
- 6.5% of those aged 12 or older in Tennessee had Substance Use Disorder
- In TN, Drug overdose deaths rates in 2021 were 56.6 per 100,000 people
- In TN, Drug overdose deaths in 2011, just 10 years earlier, rates were 17.2 per 100,000 people
- Nationally, Drug overdose deaths rates in 2021 were 32.4 per 100,000 people
Sources:
